(NEW!) The MAPIR User Guides for Program Year 2021 are available HERE.
- 2015 CEHRT Edition Required
- Security Risk Assessments in PY2021
- MU and CQM Reporting Periods
- Multiple Locations/Employers
- MU Stage 3
- Public Health Reporting for MU3
- Clinical Quality Measures
- Actions Allowable Outside the 90-Day EHR Reporting Period
You MUST be using a 2015 Edition Certified EHR System. The EHR system 2015 Edition CEHRT ID will contain “15E” in the third through fifth digits. Consult your EHR vendor if you are unsure of the certification standard of your system.
For your Meaningful Use (Promoting Interoperability) Reporting Period, you must be using a 2015 Edition CEHRT for the entire 90-day reporting period.
Security Risk Assessments in PY2021
Because of the earlier attestation window for PY2021, the requirement to complete a Security Risk Assessment (SRA) has been modified. Previously, a provider was required to attest to an SRA being completed during the PY for which they are attesting; the SRA had to already be completed prior to attestation and provide documentation of the SRA with the application.
When providers attest for PY2021, they will be asked if the measure (completing an SRA) has been completed prior to the date of attestation. If the response is "no", then they will be asked to attest that the SRA will be completed no later than December 31, 2021 and that they understand that their incentive payment will be subject to recoupment for failure to do so.
All attesting providers must upload a copy of their 2021 SRA to MAPIR by January 31, 2022, otherwise they will automatically be selected for audit.
For more information on conducting a Security Risk Assessment, please click here.
MU and CQM Reporting Periods in PY2021
- The EHR/MU reporting period is 90 days in 2021 for all providers.
- The Patient Volume reporting period is 90 days for all providers. Click here for more information.
- The Clinical Quality Measure reporting period is 90 days in 2021 for all providers.
- Attestation must be completed by July 31, 2021, therefore reporting periods must end before this date.
Those preparing and submitting applications for incentive payments in the Medicaid Promoting Interoperability Program MUST be cognizant of whether the providers they are preparing applications for practice at other locations or have other employers.
We recommend that preparers flag any provider who either:
- Practices at another location (in most instances when it is the same employer that has multiple practice sites, the CEHRT automatically combines the data, so there will likely be no extra steps needed),
OR
- Has more than one employer.
For each of these providers, you should confirm that at least 50% of their total outpatient encounters during their EHR reporting period took place at a location, or a combination of locations, with certified EHR technology (CEHRT).
Meaningful use measures can be calculated across locations and employers by adding the numerators and denominators from each CEHRT.
Please be advised that you will be putting your organization at risk of recoupment during post-payment audit if you do not consider all of the locations and employers of your attesting Providers. Furthermore, please be aware of the dates you are entering in your applications. The EHR Reporting Period should be used when completing the MU General Requirements section of the MAPIR attestation, not the Patient Volume dates.
Please refer to CMS guidance on multiple locations for further information: Guide for Eligible Professionals in the Medicaid Promoting Interoperability Program Practicing in Multiple Locations.
MU Stage 3 Objectives and Measures
Meaningful Use Stage 3 requirements have been reorganized into 8 (eight) Objectives with a total of 20 (twenty) Measures. The CMS Specification Sheets for the 2021 Medicaid Promoting Interoperability/EHR Incentive Program are posted at the CMS PY2021 webpage.
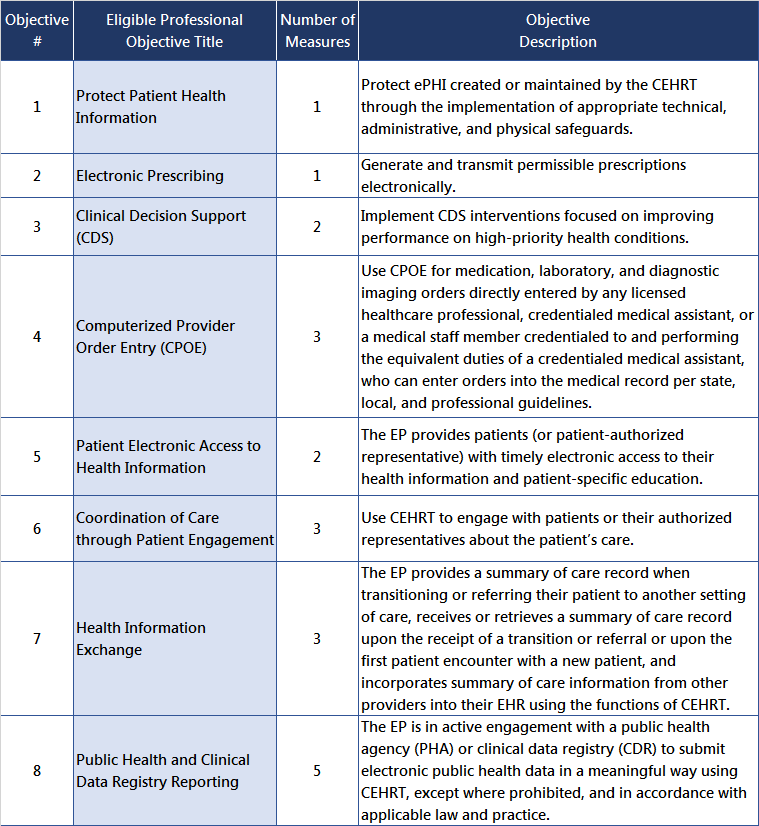
Public Health Reporting Objective in MU3
Starting in PY2020 and continuing for PY2021, important changes to the Public Health/Clinical Data Registry Reporting requirements (MU3 Objective 8) affected how Eligible Professionals selected and completed these measures. Because Vermont and New Hampshire have different Public Health registries available, Vermont and New Hampshire EPs will have different requirements for attesting to Active Engagement or for taking an Exclusion to the measures. Click the link below for the guidance and Documentation Aids for the five Public Health Reporting/Clinical Data Reporting objectives for PY2021:
PY2021 MU3 Public Health Reporting Objectives
Clinical Quality Measures for Program Year 2021
All Clinical Quality Measures in the PIP/EHR Incentive Program are referred to as "eCQMS" because they must be generated by a provider's Certified Electronic Health Record system. EPs participating in the Vermont Medicaid PIP/EHRIP are not required to submit eCQMs electronically. Click here for additional guidance: PY2021 eCQM Reporting in MAPIR (PDF, 393 KB, Updated 04/13/2021)
Examples of the MAPIR screens for PY2020 eCQM data entry are available here:
CQM_Screenshots_PY2021_MAPIR_6.4 (PDF, 5.4 MB, Updated 4/13/2021)
The CMS Promoting Interoperability website posted updates for Clinical Quality Measure reporting for Program Year 2021:
Medicaid Promoting Interoperability Program Requirements for 2021 (PDF)
Actions Allowable Outside the 90-Day EHR Reporting Period
Meaningful Use Stage 3 Objectives include measures for which action can occur before, during or after the MU reporting period of 90 days, but within the calendar year of each Program Year. Including data from the entire calendar year helps providers meet the thresholds for these measures. Each objective’s specification sheet lists the information under the ‘Additional Information’ section of any objective that allows this. In order to provide the necessary documentation to support inclusion of the data, the PIP/EHRIP Team requests a data file that verifies that the action that occurred outside the EHR Reporting period during the calendar year is valid for a patient seen during the 90-day EHR reporting period. More information can be found in this tipsheet:
ActionsAllowableOutside90DayReportingPeriod.pdf
For questions, contact the Vermont EHRIP Team at ahs.dvhaEHRIP@vermont.gov
Back to the Vermont Medicaid PIP/EHRIP Home Page
(Page last updated 04/13/2021)
