The MAPIR User Guides for Program Year 2019 are available by emailing ahs.DVHAehrip@vermont.gov
- 2015 CEHRT Edition Required
- MU and CQM Reporting Periods
- MU Stage 3
- Public Health Reporting for MU3
- Clinical Quality Measures
- Actions Allowable Outside the 90-Day EHR Reporting Period
- Updated Guidance on Objective 5, Measure 1
- Updated Guidance on Objective 7, Health Information Exchange
2015 Edition CEHRT Required
You MUST be using a 2015 Edition Certified EHR System. The EHR system 2015 Edition CEHRT ID will contain “15E” in the third through fifth digits. Consult your EHR vendor if you are unsure of the certification standard of your system.
For your Meaningful Use (Promoting Interoperability) Reporting Period, you must be using a 2015 Edition CEHRT for the entire 90-day reporting period. BUT for the Clinical Quality Measures, you do NOT need to have a 2015 Edition CEHRT for the entire 2019 calendar year. For example, if you move to a 2015 Edition Certified EHR System on July 1, 2019 and your MU reporting period is 10/03/2019 - 12/31/2019, that would meet both the MU and CQM reporting requirements.
MU and CQM Reporting Periods in PY2019
- The Meaningful Use Reporting Period is 90 days in 2019 for all providers.
- The Clinical Quality Measure reporting period is the entire calendar year 2019, unless a provider is meeting Meaningful Use for the first time in PY2019, in which case a 90-day CQM Reporting Period is allowed.
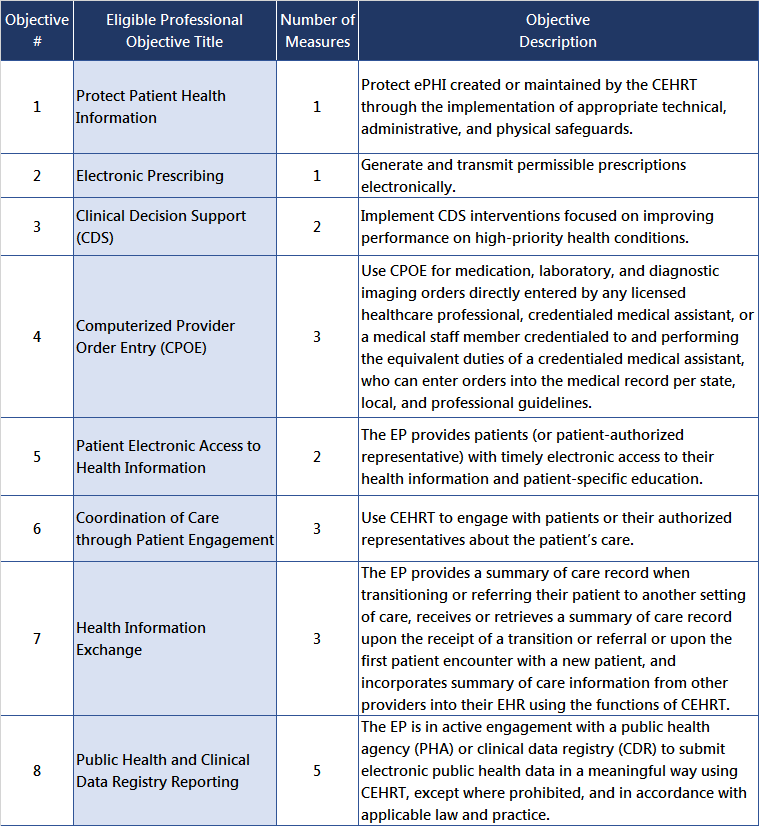
MU Stage 3 Objectives and Measures
Meanginful Use Stage 3 requirements have been reorganized into eight Objectives with a total of 20 Measures. The CMS Specification Sheets for the 2019 Medicaid Promoting Interoperability/EHR Incentive Program are posted at the CMS PY2019 webpage.
Public Health Reporting Objective in MU3
Important changes to the Public Health/Clinical Data Registry Reporting requirements (MU3 Objective 8) will affect how Eligible Professionals will select and complete the measures. Because Vermont and New Hampshire have different Public Health registries available, Vermont and New Hampshire EPs will have different requirements for attesting to Active Engagement or for taking an Exclusion to the meaures. Clink the link below for the guidance and Documentation Aids for the five Public Health Reporting/Clinical Data Reporting:
PY2019 MU3 Public Health Reporting Objectives
Clinical Quality Measures for Program Year 2019
All Clinical Quality Measures in the PIP/EHR Incentive Program are referred to as "eCQMS" because they must be generated by a provider's Certified Electronic Health Record system. EPs participating in the Vermont Medicaid PIP/EHRIP are not required to submit eCQMs electronically. Click here for additional guidance: PY2019 eCQM Reporting in MAPIR (PDF, 1.3 MB, Updated 10/16/19)
Examples of the MAPIR screens for PY2019 eCQM data entry are available here:
2019_12_06_CQM_Screenshots_PY2019_MAPIR_6.2 (PDF, 4.2 MP, Updated 12/06/19)
The CMS Promoting Interoperability website posted updates for Clinical Quality Measure reporting for Program Year 2019:
The 2019 eCQM reporting period for those who report electronically or through attestation is the full 2019 calendar year of data. For EPs attesting to Meaningful Use for the first time, the 2019 reporting period is any continuous 90-day period within CY 2019. All participating EPs are required to report on any 6 eCQMs relevant to their scope of practice from the set of 50 available. In addition, EPs must report on at least one outcome measure. If no outcome measure is relevant to his or her scope of practice, the EP must report on one high priority measure. If no high priority measures are relevant to their scope of practice, they may report on any six relevant measures. More information on each eCQM can be found on the eCQI Resource Center.
eCQM Reporting Requirement Tables
Actions Allowable Outside the 90-Day EHR Reporting Period
Meaningful Use Stage 3 Objectives include measures for which action can occur before, during or after the MU reporting period of 90 days, but within the calendar year of each Program Year. Including data from the entire calendar year helps providers meet the thresholds for these measures. Each objective’s specification sheet lists the information under the ‘Additional Information’ section of any objective that allows this. In order to provide the necessary documentation to support inclusion of the data, the PIP/EHRIP Team requests a data file that verifies that the action that occurred outside the EHR Reporting period during the calendar year is valid for a patient seen during the 90-day EHR reporting period. More information can be found in this tipsheet:
ActionsAllowableOutside90DayReportingPeriod.pdf
10/29/19 Updated Guidance from CMS on Objective 5
Objective 5 Measure 1 Application Programming Interface (API)
It has come to our attention that the language in the Stage 3 regulation and 2019 specification sheet for Objective 5, Measure 1 was unclear. Therefore, CMS has determined that in the interest of fairness, we are allowing flexibility on the requirement to meet this measure for 2019 and clarifying the requirement for 2020 in accordance with our original intention. Measure 1: For more than 80 percent of all unique patients seen by the EP:
- The patient (or the patient-authorized representative) is provided timely access to view online, download, and transmit his or her health information; and
- The provider ensures the patient’s health information is available for the patient (or patient-authorized representative) to access using any application of their choice that is configured to meet the technical specifications of the Application Programming Interface (API) in the provider’s certified electronic health record technology (CEHRT).
We understand that it is not clear that we intended the word “timely” applies to the availability of data via an API in (2), as well as the VDT in (1). The intent of this measure is that EPs must make a patient’s health data available and must offer all four functionalities (view, download, transmit, and access through API) within 48 hours of the information being available to the EP. Due to confusion, we will allow states to give EPs flexibility on meeting the second part of this measure for 2019 only. States may allow EPs to meet this measure if they:
- Have enabled an API during the calendar year of the reporting period,
- Make data available via that API for 80% of the patients seen during their reporting period,
- Provide those patients with detailed instructions on how to authenticate their access through the API and provide the patient with supplemental information on available applications that leverage the API, and
- Maintain availability of the API, i.e., it can’t be turned on for one day and then disabled.
We believe that this flexibility meets the intent of the measure while not penalizing EPs for the turbidity of the current specifications, which will be updated for 2020.
Updated Guidance for MU3 Objective 7: Health Information Exchange
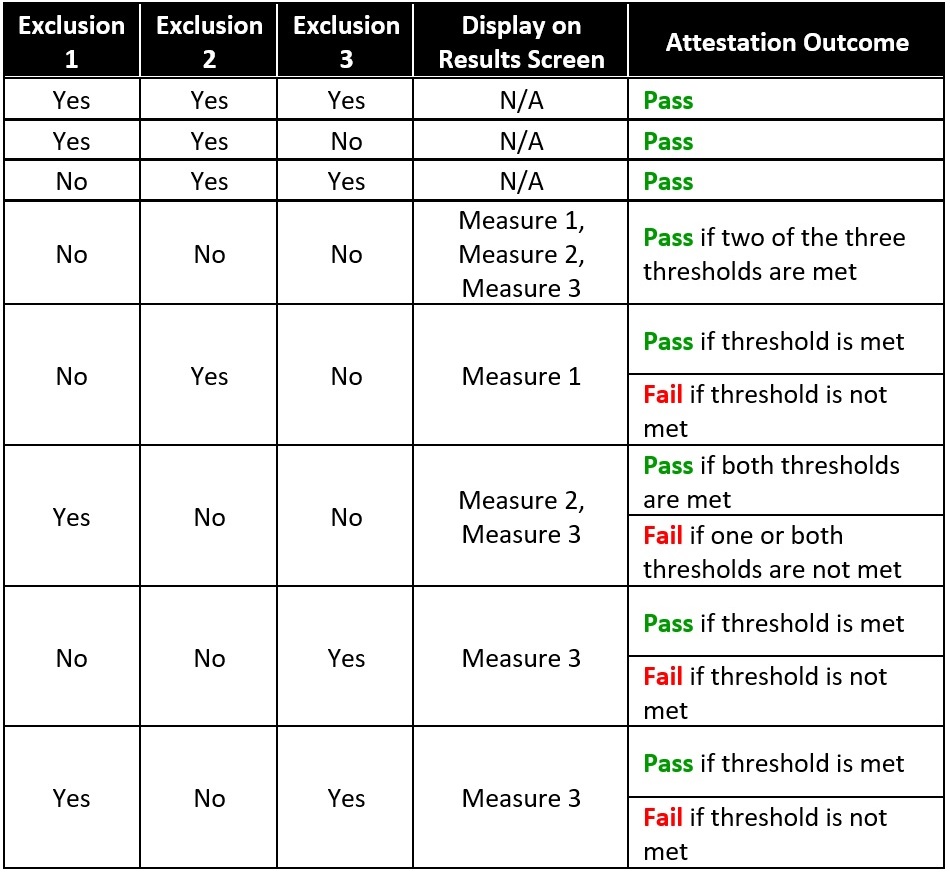
In July, CMS updated specification sheets with new criteria for EP Objective 6 and Objective 7 Meaningful Use attestation for Program Year 2019 and beyond. No modifications were required for the way MAPIR evaluates Objective 6, but the update did indicate a change for MAPIR pass/fail logic for Objective 7, Health Information Exchange, as follows:
- The objective will pass when two exclusions are taken and the threshold for the remaining measure is met.
- The objective will fail when an exclusion is selected for one measure, the threshold is met on a second measure, and the threshold is not met for a third measure.
This table displays the pass/fail outcomes of all the possible responses for Objective 7:
For questions, contact the Vermont EHRIP Team at ahs.dvhaEHRIP@vermont.gov
Back to the Vermont Medicaid PIP/EHRIP Home Page
(Page last updated 06/30/2021)