FREQUENTLY ASKED QUESTIONS
- PY2017 Attestation Availability and Deadlines
- Security Risk Analysis
- 90-Day EHR and CQM Reporting Periods
- Changes to 2017 CQMs
- Changes to MU Measures in PY2017
-
Objectives that Allow Actions Outside the 90-Day EHR Reporting Period
- Public Health Objective
- CMS Resources
- What's Next for Providers Concluding the Medicaid EHRIP
PY2017 Attestation Availability and Deadlines
The MAPIR system upgrade is complete, and providers are now able to submit their Program Year 2017 EHR Incentive Program applications. We are prepared to accept all attestations for Modified Meaningful Use Stage 2.
EXTENDED GRACE PERIOD FOR PY2017 APPLICATIONS: APRIL 30TH, 2018
The Vermont Medicaid EHRIP Team is granting an extended grace period through April 30th, 2017 for submission of Program Year 2017 attestations. In order to accommodate competing Medicare MACRA/MIPS deadlines, delays due to unexpected staffing issues, as well as technical corrections required for the data file exchanges from CMS, providers and preparers will have this extra time to finalize applications that are awaiting submission or resolution of technical issues. If you have been unable to submit Program Year 2017 applications, please reach out to the EHRIP Team for assistance as soon as possible!
Attesting to Stage 3 criteria is an option for the first time in 2017 for those providers who have upgraded their CEHRT to 2015 standards, or a combination of 2014/2015 editions that supports Stage 3. However, MAPIR will not correctly process all MU Stage 3 criteria until an additional update is applied, currently planned for August 2018. If you are planning to utilize Stage 3 Meaningful Use criteria for PY2017 applications, please contact the EHRIP Team for guidance on when to proceed: ahs.dvhaEHRIP@vermont.gov
Security Risk Analysis
Eligible professionals must conduct or review a security risk analysis for each EHR reporting period to ensure the privacy and security of their patients’ protected health information. All PY2017 attestations must include a Security Risk Analysis document that was reviewed or conducted by December 31, 2017.
For guidance and a printable SRA Tool, see our Security Risk Analysis webpage:
http://healthdata.vermont.gov/ehrip/2017/SRA
90-Day EHR and CQM Reporting Periods for Eligible Professionals
All Eligible Professionals may utilize a 90-day reporting period for both Clinical Quality Measures and Meaningful Use Objectives.
Changes to Clinical Quality Measures in PY2017
- The total number of CQMs EPs must attest to in 2017 for the EHRIP has been reduced from 9 to 6, and there are no longer any domain requirements.
- To align CQMs between Quality Payment Programs for EPs, the total number of CQMs to select from has been reduced from 64 to 53.
- Below are the 11 CQMs that are no longer active for the 2017 EHRIP for Eligible Professionals.
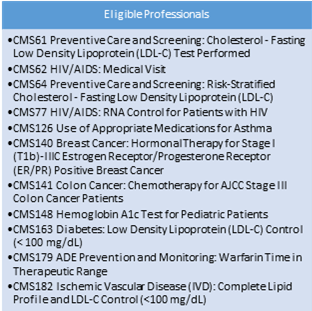
- A complete inventory of 2017 CQMs for Eligible Professionals is available at our website.
Changes to Meaningful Use Measures in PY2017
Stage 3 of Meaningful Use is an option for the first time in 2017, for those providers who have upgraded their Certified EHR Systems to the 2015 Edition, or are using a combination of 2014 and 20115 CEHRT. More information about Stage 3 criteria can be found at the CMS Website: MU3 Guidance for Medicaid EHRIP.
Most providers will still be attesting to the Modified-MU2 criteria in Program Year 2017. However, please keep in mind that certain measures and requirements have evolved for PY2017:
Changes to Specific Objectives in Modified-MU2 in PY2017
- Objective 0, ONC Questions: A CMS final rule effective 1/1/2017 requires the EP to attest to cooperating with ONC’s EHR system surveillance and review activities. Objective 0 has been added to capture this requirement. For a preview of the screenshot of the attestation questions Objective 0, click here.
- Objective 1, Protect ePHI: It is acceptable for the security risk analysis (or review of the SRA) to be conducted outside the EHR reporting period; however, the analysis must be unique for each EHR reporting period, the scope must include the full EHR reporting period, and must be conducted within the calendar year of the EHR reporting period (January 1st – December 31st).
- Objective 8, Measure 2, Patient Electronic Access: For an EHR reporting period in 2017, more than 5 percent of unique patients seen by the EP during the EHR reporting period (or his or her authorized representatives) view, download or transmit to a third party their health information during the EHR reporting period.
- Objective 9, Secure Messaging: For an EHR reporting period in 2017, for more than 5 percent of unique patients seen by the EP during the EHR reporting period, a secure message was sent using the electronic messaging function of CEHRT to the patient (or the patient-authorized representative), or in response to a secure message sent by the patient (or the patient-authorized representative) during the EHR reporting period. PLEASE NOTE that provider-initiated action and interactions with a patient, or patient-authorized representative, are acceptable for the measure and are included in the numerator.
- Objective 10, Public Health Reporting: For an EHR reporting period in 2017, all EPs must attest to at least two measures, or document exclusions if they cannot meet one or more measures. The Alternate Exclusion for Specialty Registry reporting is no longer available (“the EP did not plan to report on special registry data, therefore the EP is able to claim an exclusion”).
Objectives that Allow Actions Outside the 90-Day EHR Reporting Period
For those providers challenged to meet revised, higher thresholds for certain Meaningful Use measures in Program Year 2017, remember that the data on certain actions can be included even if the action occurred before, during or after the 90-day EHR Reporting Period (but within the calendar year). Each objective’s specification sheet lists the information under the ‘Additional Information’ section of any objective that allows this. The following objectives for Modified Stage 2 in Program Years 2017 and 2018 include this option:
•Objective 1 - Protect Patient Health Information
•Objective 5 - Health Information Exchange
•Objective 6 - Patient-Specific Education
•Objective 8 – Patient Electronic Access; Measure 2 – Patient View/Download/Transmit
•Objective 9 - Secure Electronic Messaging
In order to provide the necessary documentation to support inclusion of the data, the EHRIP Team requests a data file that verifies that the action that occurring outside the EHR Reporting period during the calendar year is valid for a patient seen during the 90-day EHR reporting period. For guidance on documenting and reporting data, please contact the Vermont Medicaid EHRIP Team: ahs.dvhaEHRIP@vermont.gov. A complete listing of Meaningful Use measures for Modified-MU2 and MU3 in 2017 and 2018 is available here: ActionsAllowableOutside90DayEHR_ReportingPeriod
Public Health Objective for Modified-MU2 in PY2017
All EPs attesting for Program Year 2017 must meet two of the three Public Health Objective Measure Options for Modified-MU2. A provider may utilize a combination of measure reporting and measure exclusions to pass the Public Health Objective. Please review the detailed guidance, screenshots and Documentation Aids available at our webpage: Public Health Reporting in PY2017 for Modified-MU2.
CMS Resources for PY2017 Requirements
- The CMS EHR Incentive Program landing page for 2017 Requirements
- Specifications and detailed additional information for Modified Meaningful Use Stage 2 Objectives and Measures
- Specifications and detailed additional information for Stage 3 MU Objectives and Measures, which are an option for the first time in PY2017
- Health Information Exchange Fact Sheet
- Security Risk Analysis Tip Sheet
- Patient Electronic Access Tip Sheet
- Public Health Reporting in 2017 for Medicaid EHRIP EPs
- 2017 Payment Adjustment Fact Sheet for EPs
Providers Concluding the Vermont Medicaid EHRIP: What's Next?
Congratulations to all those providers who have completed the six years of their eligibity with the Medicaid EHR Incentive Program! Providers finishing their incentive payments for meeting Meaningful Use in the EHRIP, please keep in mind that other quality programs still exist. For 2017 and beyond, if providers also see Medicare patients, the Merit-based Incentive Payment System will replace Medicare reporting for the Medicare EHR program, Physician Quality Reporting System and the Value-Based Payment Modifier. The Quality Payment Program is part of the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA) and includes two tracks — Advanced Alternative Payment Models (APMs) and the Merit-based Incentive Payment System (MIPS). If you have questions or need assistance with determining eligibility or requirements, visit the Quality Payment Program to find out if providers should participate in MIPS at https://qpp.cms.gov.
For questions, contact the Vermont EHRIP Team at ahs.dvhaEHRIP@vermont.gov
Back to the Vermont Medicaid EHRIP Home Page
(Page last updated 04/05/2018)
